
Plantar fasciitis is a condition that affects the fascia in the foot and causes pain. The cause of plantar fasciitis may be due to a tear or injury in the connective tissue between the heel bone and Achilles tendon. It is also related to overuse of your muscles on the bottom of your foot. Plantar fasciitis can lead to degeneration of these tissues and can cause serious damage if not treated early.
Understanding and Treating Plantar Fasciitis
Plantar Fasciitis is an extremely common and painful condition that affects millions of people worldwide. It can be caused by a variety of factors, including age, weight, activity level, and even the type of shoes you wear. If you’re suffering from Plantar Fasciitis, you know how difficult it can be to manage the pain and discomfort. But, there are a number of treatments available that are effective in relieving the symptoms of this condition. In this post, we’ll take a closer look at Plantar Fasciitis, including what it is, what causes it, and how to treat it. Whether you’re a runner, a hiker, or just someone who spends a lot of time on your feet, this guide will help you take the first step towards relief.
1. Introduction to plantar fasciitis: What is it and why is it important to understand?
Plantar fasciitis is a common condition that affects the sole of the foot and causes significant discomfort and pain. It occurs when the plantar fascia, a thick band of tissue that connects the heel bone to the toes, becomes inflamed or irritated. This inflammation can result from overuse, improper footwear, or biomechanical abnormalities.
Understanding plantar fasciitis is crucial because it can significantly impact one’s daily life and overall well-being. The pain associated with this condition can be debilitating, making simple tasks like walking or standing unbearable. It can limit mobility and prevent individuals from participating in activities they enjoy, affecting their quality of life.
Furthermore, plantar fasciitis is a condition that can persist if not properly addressed. Ignoring the symptoms or failing to seek treatment can lead to chronic pain and long-term complications. Therefore, it is essential to grasp the causes, symptoms, and treatment options available to effectively manage and overcome plantar fasciitis.
By understanding the underlying causes of plantar fasciitis, individuals can take preventive measures to minimize the risk of developing this condition. This knowledge empowers them to make informed decisions about footwear choices, exercise routines, and lifestyle habits that can contribute to the prevention and management of plantar fasciitis.
In this blog post, we will delve deeper into the intricacies of plantar fasciitis, explore its causes and risk factors, discuss common symptoms, and highlight effective treatment options. Whether you are currently experiencing the discomfort of plantar fasciitis or seeking to educate yourself for preventative measures, this comprehensive guide will equip you with the knowledge needed to step towards relief.
2. Signs and symptoms of plantar fasciitis: How to recognize the condition
Recognizing the signs and symptoms of plantar fasciitis is crucial in seeking proper treatment and finding relief. The condition primarily affects the plantar fascia, a thick band of tissue that connects the heel bone to the toes and supports the arch of the foot. Plantar fasciitis commonly occurs as a result of overuse, high-impact activities, inadequate footwear, or biomechanical issues.
One of the telltale signs of plantar fasciitis is heel pain, particularly in the morning or after prolonged periods of rest. This pain is often described as a sharp or stabbing sensation on the underside of the foot, near the heel. Some individuals may also experience pain along the arch or the entire bottom of the foot.
Another characteristic symptom is discomfort that worsens with activity. People with plantar fasciitis may notice increased pain during walking, running, or standing for long periods. The pain can be exacerbated by certain factors, such as walking barefoot, walking on hard surfaces, or wearing shoes with inadequate arch support.
In addition to pain, individuals with plantar fasciitis may experience stiffness and tightness in the affected foot. This can make it challenging to flex or bend the foot, leading to difficulty in performing activities that require mobility.
It is important to note that plantar fasciitis symptoms can vary in intensity and may develop gradually or suddenly. If you are experiencing any of these symptoms, it is recommended to consult a healthcare professional, such as a podiatrist or orthopedic specialist, for an accurate diagnosis and appropriate treatment plan.
Understanding and recognizing the signs and symptoms of plantar fasciitis is the first step towards finding relief. Early intervention and proper management can help alleviate pain, promote healing, and restore normal function to the foot, allowing individuals to regain their mobility and enjoy an active lifestyle once again.
3. Causes and risk factors: Understanding why plantar fasciitis occurs
Plantar fasciitis is a common and often painful condition that affects the foot, specifically the plantar fascia – a thick band of tissue that runs along the bottom of the foot from the heel to the toes. While the exact cause of plantar fasciitis is not always clear, there are several factors that can contribute to its development.
One of the primary causes of plantar fasciitis is repetitive strain on the plantar fascia. This can occur from activities that involve a lot of standing, walking, or running, especially on hard surfaces. People who are overweight or obese may also be at a higher risk due to the increased pressure on the feet.
Another common risk factor is having tight calf muscles and Achilles tendons. When these muscles are tight, they can put extra stress on the plantar fascia, leading to inflammation and pain. Additionally, having high arches or flat feet can also contribute to the development of plantar fasciitis.
Certain lifestyle factors can also increase the risk of developing plantar fasciitis. Wearing shoes with inadequate support or improper footwear like high heels or flip-flops can put strain on the plantar fascia. Engaging in activities that involve sudden or excessive impact on the feet, such as running or jumping, can also contribute to the condition.
Understanding these causes and risk factors is crucial in preventing and treating plantar fasciitis. By addressing the underlying issues, individuals can take steps to reduce the strain on the plantar fascia and alleviate the associated pain. This may involve wearing supportive footwear, stretching and strengthening exercises for the feet and calf muscles, and seeking professional treatment like physical therapy or orthotics.
By gaining a deeper understanding of why plantar fasciitis occurs, individuals can make informed decisions regarding their lifestyle choices and take proactive measures to prevent or manage the condition.
4. Diagnosing plantar fasciitis: How medical professionals identify the condition
Diagnosing plantar fasciitis requires a thorough assessment by medical professionals who specialize in foot and ankle conditions. While self-diagnosis is possible to a certain extent, it is always recommended to seek professional medical advice for an accurate diagnosis.
During the diagnostic process, the medical professional will start by conducting a detailed medical history review. They will ask questions about the symptoms experienced, the duration of the pain, and any previous injuries or medical conditions that may contribute to the development of plantar fasciitis.
A physical examination of the foot will also be performed. The doctor will assess the affected foot’s range of motion, check for any visible signs of inflammation or swelling, and apply pressure in specific areas to determine the pain’s exact location and intensity.
In some cases, diagnostic imaging tests may be ordered to confirm the diagnosis or rule out other potential causes of heel pain. X-rays are commonly used to assess the bony structures of the foot and rule out fractures or bone abnormalities. Ultrasound or MRI scans may also be recommended to visualize the soft tissues, such as the plantar fascia, to assess any thickening or tears.
It is important to note that the diagnosis of plantar fasciitis is often a clinical one, meaning that it is based primarily on the patient’s symptoms and physical examination findings. Medical professionals rely on their expertise and knowledge to accurately identify the condition and differentiate it from other similar foot conditions.
Once a diagnosis of plantar fasciitis is confirmed, appropriate treatment options can be recommended to alleviate pain, promote healing, and prevent further complications.
5. Treatment options: Conservative approaches to alleviate pain and promote healing
When it comes to treating plantar fasciitis, conservative approaches are often the first line of defense. These methods focus on alleviating pain and promoting healing without the need for surgical intervention. While every case is unique, there are several tried and true treatment options that have shown promising results.
One of the most common conservative treatments for plantar fasciitis is stretching exercises. These exercises aim to stretch the tight muscles and tendons in the foot and calf, relieving tension on the plantar fascia. They can include simple stretches like toe curls, calf stretches against a wall, or the use of a towel to stretch the arch of the foot.
Another effective treatment option is the use of orthotic inserts or shoe inserts. These inserts provide additional arch support and cushioning, helping to distribute pressure evenly across the foot and reduce strain on the plantar fascia. They can be purchased over-the-counter or custom-made to fit the specific needs of the individual.
In addition to stretching and orthotics, physical therapy can also play a key role in the conservative treatment of plantar fasciitis. A physical therapist can guide patients through targeted exercises and techniques to improve flexibility, strengthen the foot and leg muscles, and promote proper biomechanics. They may also incorporate modalities such as ultrasound or electrical stimulation to aid in pain relief and tissue healing.
Other non-invasive treatments that can provide relief include the use of night splints, which help to stretch the plantar fascia and Achilles tendon while sleeping, and the application of ice or cold therapy to reduce inflammation.
It’s important to note that conservative treatments may take time to show significant improvement, and a combination of approaches is often necessary for optimal results. However, by diligently following these methods, many individuals with plantar fasciitis are able to find relief and prevent further progression of the condition.
6. Stretching exercises for plantar fasciitis: A step-by-step guide
Stretching exercises can play a crucial role in relieving the pain and discomfort caused by plantar fasciitis. These exercises aim to stretch and strengthen the muscles and tendons in the foot, providing much-needed relief and promoting healing.
Before diving into the step-by-step guide, it’s important to note that stretching exercises should be performed gently and gradually. Overstretching or pushing too hard can aggravate the condition and cause further damage. Listen to your body and stop if you experience any pain or discomfort during the exercises.
Here are some effective stretching exercises for plantar fasciitis:
1. Calf Stretch:
– Stand facing a wall, with one foot in front of the other.
– Lean forward, placing your hands on the wall for support.
– Keep the back leg straight and the heel on the ground, while bending the front knee.
– Hold this position for 30 seconds, then switch legs and repeat.
2. Plantar Fascia Stretch:
– Sit on a chair and cross one leg over the opposite knee.
– Using your hand, gently pull back the toes towards the shin until you feel a stretch in the arch of the foot.
– Hold this stretch for 15 to 30 seconds, then release and repeat on the other foot.
3. Toe Stretch:
– Sit on the floor with your legs extended in front of you.
– Place a towel or resistance band around the ball of your foot.
– Gently pull back on the towel or band, flexing your toes towards your body.
– Hold the stretch for 15 to 30 seconds, then release and repeat.
4. Achilles Tendon Stretch:
– Stand facing a wall, with one foot in front of the other.
– Lean forward, placing your hands on the wall for support.
– Bend the back knee slightly, keeping the heel on the ground.
– Hold this position for 30 seconds, then switch legs and repeat.
Remember to perform these stretches daily, ideally multiple times a day, for optimal results. Additionally, it’s important to combine these exercises with other treatments recommended by your healthcare professional, such as wearing supportive shoes, using orthotic inserts, or undergoing physical therapy.
By incorporating these stretching exercises into your daily routine, you can take a proactive approach towards relieving the symptoms of plantar fasciitis and promoting the healing process. However, if the pain persists or worsens, it is always advisable to consult with a healthcare professional for a comprehensive diagnosis and personalized treatment plan.
7. Footwear considerations: Choosing the right shoes to support your feet
When it comes to managing and treating plantar fasciitis, one crucial aspect to consider is your footwear. The shoes you wear play a significant role in supporting your feet and alleviating the symptoms of this condition.
First and foremost, it is essential to opt for shoes that provide excellent arch support. Plantar fasciitis often occurs due to excessive stress on the plantar fascia, the ligament that supports the arch of the foot. By choosing shoes with proper arch support, you can help distribute the weight evenly and reduce strain on the ligament.
Additionally, look for shoes with a cushioned sole. A well-cushioned shoe can help absorb shock and decrease the impact on your feet while walking or running. This can be particularly beneficial for individuals who have plantar fasciitis, as it can help reduce pain and discomfort.
Another factor to consider is the shoe’s stability and motion control features. Shoes with good stability can help control excessive foot motion, which can contribute to the development or worsening of plantar fasciitis. Look for shoes with a firm heel counter and a supportive midsole to provide stability and prevent overpronation.
Furthermore, ensure that the shoes you choose have a spacious toe box. A cramped toe box can put additional pressure on the toes and aggravate the symptoms of plantar fasciitis. Opt for shoes that allow your toes to move comfortably and freely.
It is advisable to avoid high heels or shoes with minimal support, as these can exacerbate the condition. Instead, prioritize comfort and functionality over fashion when selecting footwear for plantar fasciitis.
Remember, everyone’s feet are unique, and what works for one person may not work for another. It is recommended to try on different shoe brands and styles to find the ones that provide the best support and comfort for your feet. Consider consulting with a podiatrist or footwear specialist who can guide you in selecting the right shoes to alleviate the symptoms of plantar fasciitis and promote proper foot health.
8. Physical therapy and other interventions: Advanced treatment methods for chronic cases
When it comes to chronic cases of plantar fasciitis, physical therapy and other interventions can be highly effective in providing relief and promoting healing. These advanced treatment methods go beyond the basic home remedies and conservative measures commonly utilized for milder cases.
Physical therapy plays a crucial role in the management of chronic plantar fasciitis. A skilled physical therapist will assess the underlying causes of the condition and develop a personalized treatment plan to address them. This may involve a combination of exercises to stretch and strengthen the muscles and tissues in the foot and lower leg, as well as techniques to improve flexibility, balance, and gait mechanics. Additionally, the therapist may utilize modalities such as ultrasound, electrical stimulation, or manual therapy to further alleviate pain and inflammation.
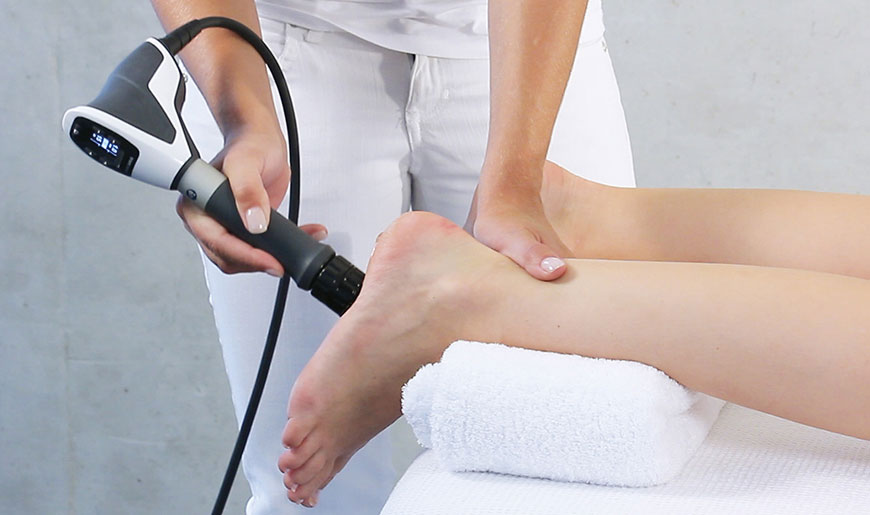
In some cases, extracorporeal shockwave therapy (ESWT) may be recommended as an adjunct to physical therapy. This innovative technique involves the use of high-energy sound waves to stimulate healing and reduce pain. ESWT has shown promising results in the treatment of chronic plantar fasciitis by targeting the affected tissues and promoting the regeneration of healthy cells.
Another intervention that can be considered for chronic cases is corticosteroid injections. These injections deliver a powerful anti-inflammatory medication directly into the affected area, providing rapid pain relief. However, it’s important to note that this intervention is typically used as a short-term solution due to potential side effects with long-term use.
In more severe cases that have not responded to conservative measures, surgical options may be explored. These can range from minimally invasive procedures, such as plantar fascia release, to more extensive interventions involving the removal of bone spurs or the repair of damaged tissues. Surgery is generally considered a last resort and is only recommended when all other treatment options have been exhausted.
It’s worth noting that the choice of intervention for chronic plantar fasciitis should be made in consultation with a healthcare professional experienced in foot and ankle conditions. They will take into account the severity and duration of the symptoms, as well as individual factors like age, lifestyle, and overall health, to determine the most appropriate course of action.
By seeking out advanced treatment methods such as physical therapy, ESWT, or surgical interventions when necessary, individuals with chronic plantar fasciitis can take significant steps towards finding lasting relief and improving their quality of life.
9. Preventing plantar fasciitis: Tips for maintaining foot health and reducing the risk of recurrence
Preventing plantar fasciitis is crucial in maintaining foot health and reducing the risk of recurrence. By implementing a few simple tips and habits, you can take proactive steps towards keeping your feet strong and pain-free.
First and foremost, it is essential to wear proper footwear that provides adequate support and cushioning. Invest in shoes that are specifically designed for your foot type and activity level. Avoid unsupportive or worn-out shoes that can strain the plantar fascia and lead to injury.
Maintaining a healthy weight is also important in preventing plantar fasciitis. Excess weight puts additional pressure on the feet, increasing the risk of developing foot problems, including plantar fasciitis. Incorporating regular exercise and a balanced diet can help in achieving and maintaining a healthy weight.
Stretching and strengthening exercises can play a significant role in preventing plantar fasciitis. Regularly stretching the calf muscles and the plantar fascia itself can help improve flexibility and reduce tension in the foot. Strengthening exercises focusing on the foot and ankle can also help in supporting the arch and preventing excessive strain on the plantar fascia.
Avoiding activities that place excessive stress on the feet is another preventive measure. High-impact sports and activities that involve repetitive motions can increase the risk of developing plantar fasciitis. If engaging in such activities, ensure proper warm-up, cooldown, and adequate rest days to allow the feet to recover.
Maintaining good overall foot hygiene is often overlooked but important in foot health. Keeping the feet clean and dry, wearing breathable socks, and rotating shoes can help prevent fungal infections and reduce the risk of foot-related complications.
Lastly, listening to your body and addressing any foot discomfort or pain promptly is crucial. Ignoring early signs of plantar fasciitis can lead to a more severe condition. If you experience persistent foot pain, consult a healthcare professional for an accurate diagnosis and appropriate treatment.
By incorporating these preventive measures into your daily routine, you can significantly reduce the risk of developing plantar fasciitis and maintain optimal foot health. Remember, taking care of your feet is a proactive step towards overall well-being and a pain-free lifestyle.
10. Living with plantar fasciitis: Coping strategies and support for those managing the condition
Living with plantar fasciitis can be a challenging experience, but there are coping strategies and support available to help you manage the condition. Here are some tips to help you navigate through the daily challenges of living with plantar fasciitis.
1. Seek professional help: It’s crucial to consult a healthcare professional, such as a podiatrist or orthopedic specialist, who can provide an accurate diagnosis and develop a personalized treatment plan for you. They can also offer guidance on managing pain and recommend appropriate footwear or orthotics.
2. Modify your activities: While it’s important to stay active, certain high-impact activities like running or jumping may exacerbate the pain. Consider low-impact exercises like swimming or cycling to maintain your fitness level without putting excessive strain on your feet.
3. Stretch and strengthen: Regular stretching exercises can help alleviate tightness in the calf muscles and the plantar fascia. Strengthening exercises for the muscles in your feet and lower legs can also provide stability and support. Your healthcare professional can recommend specific exercises tailored to your condition.
4. Wear supportive footwear: Invest in shoes that provide proper arch support, cushioning, and stability. Avoid flat shoes or those with worn-out soles, as they can aggravate the symptoms. Orthotic inserts or custom-made shoe inserts may also be beneficial in providing additional support.
5. Ice and massage: Applying ice to the affected area can help reduce pain and inflammation. Additionally, massaging the plantar fascia and surrounding muscles can help improve circulation and alleviate discomfort.
6. Pain management techniques: Over-the-counter pain relievers, such as non-steroidal anti-inflammatory drugs (NSAIDs), can help manage pain and reduce inflammation. However, it’s important to consult with your healthcare professional before starting any medication.
7. Seek support: Living with a chronic condition like plantar fasciitis can take an emotional toll. Reach out to support groups or online communities where you can connect with others facing similar challenges. Sharing experiences and tips can provide valuable emotional support and coping strategies.
Remember, everyone’s experience with plantar fasciitis is unique, and what works for one person may not work for another. It’s important to listen to your body, be patient with the healing process, and collaborate with your healthcare professional to find the best strategies for managing your condition. With the right support and coping strategies, you can minimize the impact of plantar fasciitis on your daily life and take steps towards relief.
